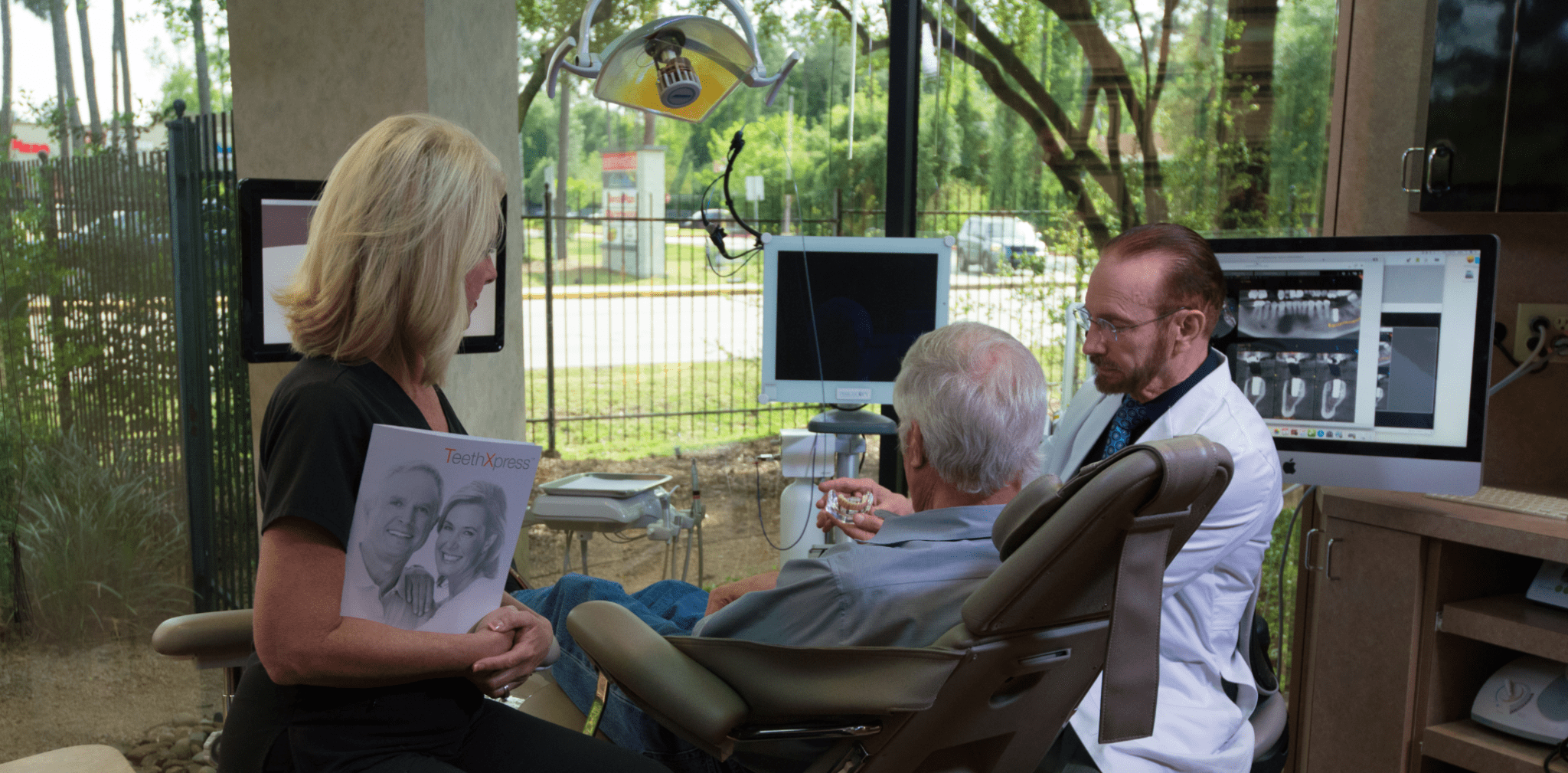Crown Lengthening
Tooth Extraction Conroe
Tooth Extraction the Woodlands
Cosmetic Dentist Conroe
Cosmetic Dentist the Woodlands
Laser Gum Therapy
TeethXpress
Dental Implants Conroe
Dental Implants the Woodlands
Premier Dental Implants in The Woodlands
GREATER NORTH HOUSTON-SPRING-THE WOODLANDS-HUNTSVILLE
Dr. Saunders and Dr. Sajadi, with office locations in The Woodlands, TX started placing dental implants in 1986 and has placed over 7,000 implants with excellent results. Dental implants or tooth implants can be used to replace individual and are also used to support full dentitions like with TeethXpress, which effectively delivers a brand new fully functioning set of beautiful teeth where dentures or compromised teeth were before. All patients wanting dental implants in The Woodlands areas can conveniently make their complimentary appointment at either location online or by phone.
Naturally Pleasing Aesthetics
Restore your smile with implants that look like your natural teeth.
Naturally Beautiful Form
Preserve facial contours and jaw bone that would otherwise recede and deteriorate with missing teeth.
Naturally Strong Function
Regain the ability to eat virtually anything with confidence.
Affordable Financing Options
Explore multiple financing options for restoring your smile.
The Periodontal Center of Excellence Dental Implant Benefit
A Beautiful Transformation of Your Smile & Confidence
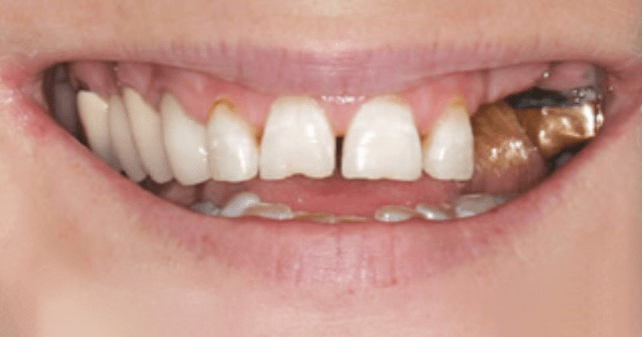
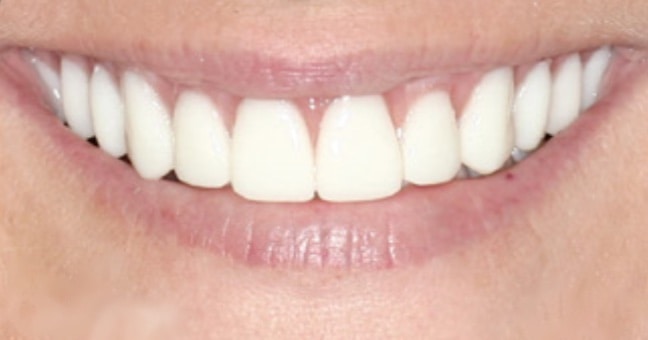
Dr. Saunders, Dr. Sajadi, and the PCE Team make your dental implant experience simple, affordable, and with the highest quality of care. You can always count on:
- Latest Dental Implant Technology & Innovation
- Most Comfortable Experience Possible
- Over 30 Years of Experience
- Highly Trained and Attentive Staff
- Multiple Financial Options
Your dentist will talk to you about your cosmetic goals and concerns, answer any questions you may have, and discuss your treatment options. Your dentist will likely also perform a thorough dental exam and health history review. If your dentist notices any issues that you do not mention, they will be sure to talk to you about those as well.

Cosmetic dentistry can correct a wide range of problems, including chipped, cracked, or misshapen teeth, gaps or spaces between teeth, misshapen or misaligned teeth, yellow or discolored teeth, teeth that are too small or large, overlapping or crooked teeth, etc. It also treats excessively worn teeth and those with abnormal alignment.
Our The Woodlands Implant dentist primarily uses titanium implants. Titanium is extremely strong, resistant to corrosion (which is important since it’s constantly exposed to saliva), lightweight, hypoallergenic for people with metal sensitivity or allergies, and is the color of silver. New developments are being worked out to create durable, predictable ceramic dental implant designs. Since ceramics are tooth colored, they eliminate some aesthetic concerns associated with possible implant exposure. But a great periodontist in The Woodlands can still place a custom ceramic crown over traditional titanium implants to keep them looking great! Let our The Woodlands Implant dentist know if you have specific smile makeover goals that you want to achieve, as titanium is still the best implant material available.
Replacing one missing tooth used to mean getting a dental bridge attached to two healthy teeth on either side of your missing one. If you have healthy enamel, it would need to be ground down so that a bridge could fit over it.
Single tooth dental implants are non-invasive to other teeth, helping you protect your healthy smile and avoiding unnecessary tooth alteration.
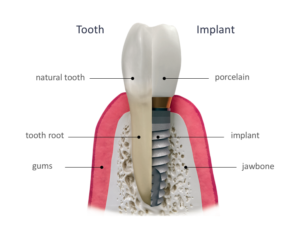
With individual tooth replacement, an implant is set into the location of the missing tooth. On top, an abutment extends through the gums and into your mouth, providing a base for the fixed restoration. Then, a Periodontist in The Woodlands attaches a porcelain crown on top of the abutment, finishing off the overall unit.
When you smile in the mirror, your single tooth implant and crown blend in with all of your other teeth! And the best part is that no other teeth had to be altered in the process.
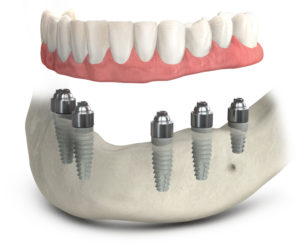
Many people who are missing several teeth or wear fixed-bridges, removable partial-dentures or conventional dentures don’t like the way they look or function. The TeethXpress procedure offers a much better solution to achieving an attractive, natural looking smile. Your dental implant supported teeth will allow you to eat your favorite foods again and go about your daily life with confidence! Dr. Saunders and Dr. Sajadi are Certified TeethXpress providers and can help determine if the TeethXpress procedure is the solution for you. With a complimentary 3D Scan, exam, and financial consult the PCE Team will provide everything you need for you to make the decision that is right for you.
AWith our TeethXpress option, you can enjoy the benefits of dental implants across your entire smile. This fast implant treatment provides full mouth restoration when you need to replace all of your teeth at one time.
The functional and design benefits of dental implants mean that your permanent prosthesis will be more comfortable than wearing a removable denture. Instead, you’ll have a streamlined hybrid device that never slips out of place and won’t cover the roof of your mouth. That way it’s easier to talk and enjoy the flavors of all your favorite foods!
Absolutely. Since the cost of dental implants varies depending on your unique situation and insurance coverage, flexible payment plans make it easier to budget your procedure at an affordable monthly rate.
Usually the cost of dental implants can be financed at 0% or a very low interest rate for terms up to 12-18 months at a time. That way you can start treatment as soon as you’re ready and immediately begin enjoying the perks of a strong, new smile.